An emergency medicine physician fighting Covid-19 in Boston
Elizabeth Temin ’86, M.D., M.P.H., is an attending physician at the Massachusetts General Hospital Department of Emergency Medicine in Boston. She is also an assistant professor in the Department of Emergency Medicine at Harvard Medical School.
When we spoke with Liz Temin ’86 in mid-April, she had completed a shift in Mass General’s emergency department just the day before; 140 intensive-care patients were on ventilators that day, compared with an average of 57. Covid-19 patients now fill around one third of the 1,000-bed hospital, which has canceled nearly all elective procedures. Orthopedists and other medical specialists are helping to staff the emergency department to free emergency attendings to work in the hospital’s the 10 intensive-care units. (Their number has increased: For example, a postoperative recovery area has been converted into an additional ICU, and a pediatric ICU has been repurposed for adults.)
“It’s a big hospital with a lot of resources,” Temin says. “Everybody has been doing an amazing job mobilizing. We’re able to handle a lot.” Although the Covid-19 hospitalization peak was anticipated last week, Temin says the effectiveness of social distancing may mean that the curve is being not only flattened but also elongated. It’s difficult to know, day to day, when the worst may pass.
The influx of patients is not the only challenge the pandemic poses for medical providers. Whereas most patients needing treatment for pneumonia require ventilation for four or five days, Covid-19 patients may stay on vents for two or three weeks. “Cumulatively, our resources are strapped, even if we’re able to handle momentary surges,” Temin says. “The surges don’t seem to end. They just build on each other.”
In response to the nationwide shortage of personal protective equipment, hospital partners recently introduced a new process to sterilize N95 masks for reuse, and no one at Mass General has had to go without masks or gowns or gloves. Now, though, Temin wears one N95 mask throughout an entire shift, rather than one per patient as usual. In full protective gear, it’s hard to hear anyone, Temin says: “It’s muffled, and that hinders the personal portion of patient care, which is sad.”
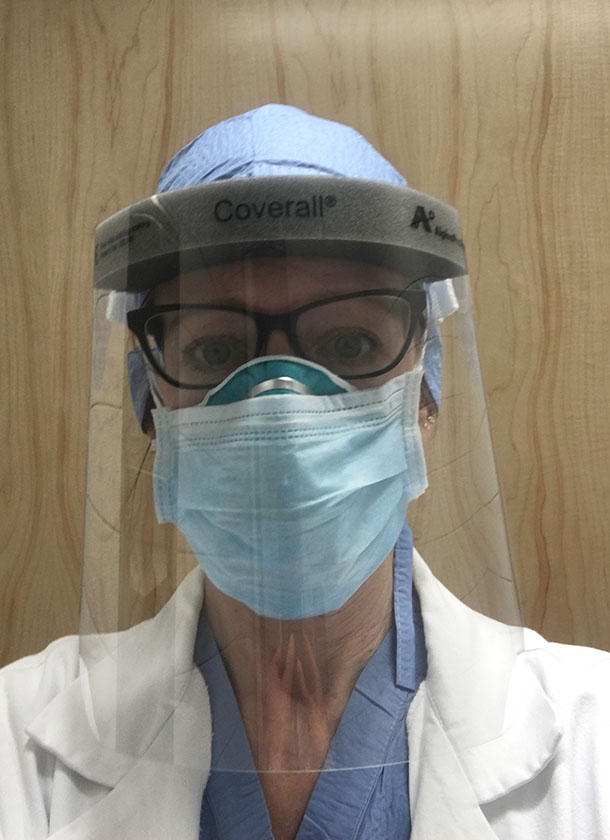
“Shifts are exhausting and stressful, but I get to come home and have a little down time with my family to recover.”
– Elizabeth Temin ’86
The time she spends at home keeps Temin going. “Shifts are exhausting and stressful, but I get to come home and have a little down time with my family to recover,” she says. Though coming home, in itself, is much more difficult than it used to be. Many of Temin’s colleagues are very concerned about infecting their families, and some are self-isolating from them. Temin’s husband is also a physician, so before coming home to each other and their teenage sons, they both follow extensive routines: changing into separate clothes at the hospital, careful handwashing, and wearing gloves, then repeating the process when they come home — changing before entering the house and showering before touching anything.
Quarantining with her family has been an unexpected upside for Temin, who has relished the additional contact with her children. “Teen boys don’t usually want to spend a lot of time with their mothers,” she says. “We’ve been eating meals and watching movies together. I’m amazed it’s gone as well as it has. It’s been lovely.”
One of the activities they all individually enjoy is reading, a passion that dates back to Temin’s time at CA. “CA really shaped who I am as a person, what I think is interesting, how I relate to the world and to other people, and how I want to portray myself,” Temin says. She credits the leadership of female teachers at CA as a model for navigating the challenges of being a strong professional woman.
“We’re a very short-term nation, focused on the next election. And for this pandemic, there has to be a long-term intervention.”
– Elizabeth Temin ’86
Temin didn’t always want to be a physician. At CA, she loved art, literature, theater, and math, but avoided studying science. In college, she majored in literature and music. It wasn’t until years later, when volunteering at Boston’s Museum of Science, that she found her calling. “I ended up dissecting eyeballs there,” she says, “and realized it was the coolest thing.” A post-baccalaureate program at Harvard followed, as did laboratory work, and eventually her career in medicine. Temin received her medical degree from Albert Einstein College of Medicine, then completed her residency in emergency medicine at Boston Medical Center and a fellowship at Boston Emergency Medical Services and Boston Medical Center.
When medical providers are thanked these days, Temin admits it makes her embarrassed. “The best way people can honor us is to social distance and take care of themselves,” she says. “Quit smoking, try to lose weight so you don’t have adult-onset diabetes — all those things that make you a higher risk when you get sick.”
The medical community has learned a lot from smaller epidemics — SARS, MERS, and Ebola — Temin says, but she adds that “our government hasn’t been willing to take the steps needed to protect our nation. Our country has dismantled so many of the safety nets that would have helped in this crisis.” She points not only to public health but also to services such as food assistance and transit systems that so many rely on. “We’re a very short-term nation, focused on the next election,” Temi says. “And for this pandemic, there has to be a long-term intervention.”
She is particularly concerned about the erosion of belief in and support of medical research in the United States that may make some people wary of any eventual vaccines, and conspiracy theories that are circulating. “The country we’ve created over time is so mistrustful, and there’s so much false news out there, that it can be hard for people to know what’s true,” Temin says. “If you can’t get real information, you don’t know how to act.”
For now, Temin takes refuge in her family. And while she’s keenly aware of the damage already done to the country’s social fabric, she sees glimmers of hope. “It’s amazing how everybody has really pulled together and is willing to really help each other — in terms of the national response but also regular people helping neighbors get groceries,” she says. “I hope that attitude of being on the same team is something that we can continue. Will this be enough to repair the damage that’s been done?”